This stillborn infant was delivered vaginally to his 30 year old, primigravida mother at 33 weeks of gestation. Mother’s medical history includes hypothyroidism and gestational diabetes. Ten days before fetal death was detected the biophysical profile was 8/8, and the AFI 18. Intrauterine fetal death was confirmed by ultrasound examination at 9:15 AM. Her glucose at 11 AM on that day death was 134 g/dl. Her BMI was 39.16.
The autopsy external examination was consistent with 33 weeks of gestation. Persistent nephrogenesis was also indicative of less than 36 weeks of gestation (Fig 1). The infant was large for that gestation (2,520 grams).
The infant externally had collapsed skull bones and extensive desquamation. Based on Genest criteria of some loss of bronchial basophilia (Fig 2), and complete loss in the liver, but retained cartilage basophilia (Fig 3), intrauterine retention was between 3 and 7 days.
The infant had increased thoracic subcutaneous (0.7-1 cm), pericardial and perirenal adipose tissue for gestational age (Fig 4,5). The cheeks were very full. The heart appeared large in the chest (Fig 4A). By weight the liver and heart were relatively heavy compared to the thymus, adrenals and kidneys (Fig 6). However the lungs and spleen were also relatively heavy. There was erythroblastosis (Fig 7). Despite marked autolysis the islets did appear to have cytomegaly and an inflammatory infiltration (Fig 8). The heavy for gestation infant with full cheeks, erythroblastosis, increased adipose tissue, a large heart, and likely islet cell hypertrophy and inflammation are typical of an infant of a diabetic mother.
There were moderate pleural effusions and ascites.
There was no gross or microscopic evidence of thyroid tissue (Fig 3). Because the neck organs are removed just above the hyoid bone, sublingual thyroid tissue cannot be excluded. The parathyroids were present (Fig 8). There was no evidence of scarring, suggesting that this was a primary thyroid aplasia rather than a maternal anti-thyroid antibody. There was histologic evidence of some thymic involution with increased surrounding adipose tissue (Fig 9), but this was not marked.
This infant died not long after a normal biophysical profile. The effusions suggested a relatively brief period of cardiac failure. The most striking findings were the absent thyroid, and extreme adipose deposition for 33 weeks of gestation. Congenital hypothyroidism is not a known cause of stillbirth. The thyroid in utero does not secrete active hormone but mostly reverse T3. This is not surprising since the infant is surrounded by a body temperature water bath. Yet, the extreme adipose tissue deposition could be a consequence of decreased energy metabolism in an infant who because of mass effect (Pederson hypothesis) receives increased glucose, and therefore might have more fat deposition than the normal thyroid infant of a diabetic mother.
The history did not include any evaluation of why the mother was hypothyroid, and whether her high BMI was related to that disease. There is very little published anatomic literature on absent thyroid, the only cited autopsies are in an old German publication (Die Entwicklungsstorungen Schilddruse in a 1937 book) which notes that parathyroids are normally present as they are in this case. Most of the features of severe congenital hypothyroidism such as the immature facies and open fontanels would be difficult to detect in this autolytic premature infant of a diabetic mother.
No cause of death could be determined, but the combination of maternal diabetes and fetal absent thyroid could have compounded adverse metabolic consequences on glucose metabolism.
Figure 1 Kidney: There is still some basophilic nuclear staining beneath the capsule which shows more primitive collections of cells from continuing nephrogenesis, a process that is usually complete by 36 weeks of gestation.

Figure 2 Lung: The bronchus demonstrates unanchored bronchial epithelial cells in the lumen, a few of which have lost nuclear basophilia. The remaining lung does not show marked congestion of vessels nor aspirated meconium to account for a heavy weight.


Figure 3 Neck: Multiple neck samples were taken and these had multiple levels examined, and no thyroid could be identified. There was very prominent peritracheal adipose tissue. There is still basophilia of the cartilage cells.

Fig 4: The open chest demonstrates the thick subcutaneous adipose tissue, the pleural effusions, and a not particularly small thymus.

Fig 4A: The exposed heart appears to have a large dilated right ventricle, and overall to be large.
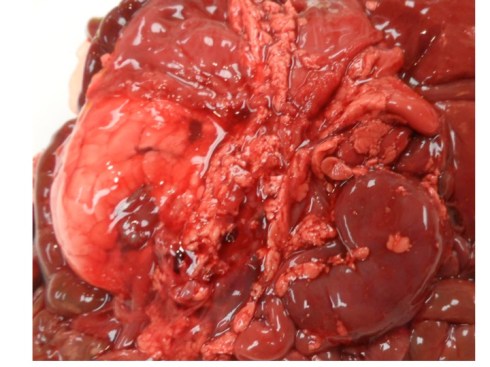
Fig 5: The kidney on the left demonstrates the perinephric fat which has been stripped from the kidney on the right. The adrenal on the right does not look small, but in general the fetal adrenal should appear somewhat larger compared to the kidney. The left adrenal is still covered by diaphragm.

Fig 7: Umbilical cord blood showing increased nucleated red cells (dark very round nuclei with a halo of red cell)

Fig 8 pancreas: The autolysis of the pancreas makes interpretation less certain. The blue arrows point to eosinophils that are often found in the lists of infants of diabetic mothers. The black arrow points to a very large nucleus that is consistent with beta cell hypertrophy but artifact from the autolysis makes that diagnosis uncertain.

Fig 9 thymus: The lobules do have a small isolated appearance between connective tissue adipose, but in the large lobules the ratio of cortex to medulla is not markedly reduced.

Fig 8: This is a graph of each organ:brain weight ratio divided by the expected organ:brain weight ratio. This normalizing procedure usually produces an easily interpretable pattern in IDM stillbirths, with a large heart and a large liver, or if there is an anomalous weight the cause can be determined by the histological changes. I checked the entry of the weights into the spread sheet and they were correct. I have no good explanation for the high lung and spleen weights in this case.
Leave a comment