This stillborn male infant was delivered by precipitous vaginal delivery at 33 weeks of gestation to his 30 year old, G3, Term 2, Living 2, Afro-American mother. Birth weight was 1,630 g. The mother’s prenatal care was unremarkable. She is blood type O+. The discharge summary diagnosed preeclampsia and dehydration. There was no Kleihaurer Bedtke test to detect fetal maternal hemorrhage, but a differential blood count on the mother after delivery had zero nucleated red cells.
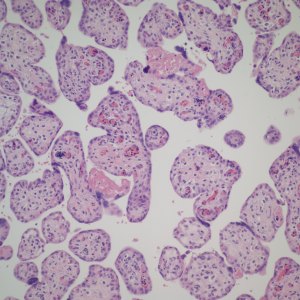
The placental examination demonstrated a marked erythroblastosis (Fig 1). There was mild hydrops. There were no intranuclear inclusions typical of Parvo virus in the nucleated red blood cells, and an immunostain for Parvo virus was negative.
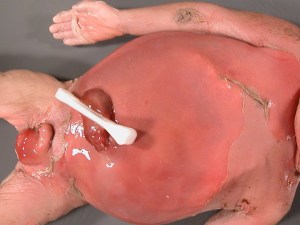
The external examination demonstrated a hydropic male infant with prolonged retention based on extensive desquamation, and collapsed skull bones. However, the umbilical cord and abdomen were a pale pink, rather than the expected deep red (Fig 2). The gestational age exam demonstrated plentiful lanugo, 3-4 mm flat areola, descended testes, and slow recoil of the pinna. There were no plantar creases and no visible vessels, but these were not accurate parameters of gestation as the former appeared due to hydrops and desquamation and the latter due to the pallor. By cheating on the physical Ballard score, and giving 1 for both skin and plantar creases, the gestation is between 29 and 30 weeks, and giving 2 both for skin and plantar creases yields 32 weeks. The infant weighed 1,420 g at autopsy with loss of subcutaneous fluid weight into the blankets which likely accounts for the difference from the birth weight. The autopsy weight is appropriate for this range of gestations. There were no malformations.
Fig 2 Infant showing extensive desquamation and pale red color of abdomen and cord
The internal examination demonstrated only small pleural effusions. The thymus appeared small and the spleen large. The heart was normal but the ductus arteriosus appeared relatively narrow but still more than 50% of the descending aortic diameter. The brain was very soft but not liquid and the convolution development was appropriate for 30-32 weeks of gestation. There were no malformations of any organ.
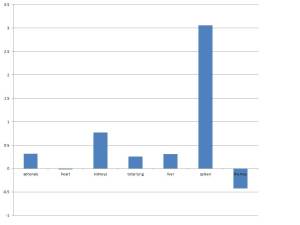
The weights are listed in table 1. Since the relative weights are usually most informative, I have calculated the organ to brain weight ratios and then subtracted these from the expected ratios, then divided that difference by the expected ratio[1]. The graph of this calculation makes interpretation of the weights easier (Fig 3). The kidney and spleen are clearly larger than they should be. The heavier adrenals and lighter thymus are consistent with stress, adrenal lipid accumulation and thymic loss of cortical lymphocytes, but not very marked. The lungs are not small, as would be expected had there been a persistent pleural effusion and this result correlates with the small effusion and normal lung size seen grossly.
Table 1
Autopsy
weight Brain Lungs Heart Kidneys Adrenals Liver Spleen Thymus
1420 270 52.8 14.1 33.0 7.8 113.3 24.1 4.2
The microscopic evaluation of intrauterine postmortem retention based on the publication of Genest and colleagues was at least one week with complete loss of basophilia in the liver, adrenal and ileocecal sections, and loss of tracheal cartilage basophilia[2]. The external features did not appear to be extreme and the kidney was microscopically relatively intact, suggesting that in the more than 1 week to less than 4 week Genest interval of dating, this infant was closer to the one week.
The thymus showed a modest loss of cortex microscopically and the adrenal could not be easily evaluated, and there was no frozen sample for fat staining, but the findings were not those of prolonged fetal stress as would have been expected in Rh alloimmunization. The kidney interstitium demonstrated plentiful hematopoiesis which appeared to account for the increase in weight. As is typical in the kidney, the hematopoietic response included myelopoiesis (Fig 4). The enlarged spleen was due to a cellular infiltration not just congestion, but the autolysis compromised interpretation. An iron stain highlighted a diffuse distribution of hemosiderin macrophages that were no very evident on H&E stain (Fig 5).

[caption id="attachment_58" align="alignnone" width="300"] Spleen, left H&E 20x, right iron stain 40s showing pale hemosiderin macrophages.
Spleen, left H&E 20x, right iron stain 40s showing pale hemosiderin macrophages.
Kidney showing hematopoiesis around a vessel, H&E 20x[/caption]
The placenta had a mild maternal chorioamnionitis and despite an absence of neutrophils in the fetal lung or stomach, postmortem lung cultures grew scant Corynebacterium species. This inflammation was likely postmortem from the fetal perspective, but may have facilitated the onset of labor.
The underlying diagnosis in this infant was a relatively acute onset of hydrops related to a drop in hematocrit and likely high output heart failure, based on the marked erythroblastosis in the placenta, and the pale edematous fetus.
There are four main differential considerations of the cause.
1. Hemorrhage: There was no internal hemorrhage. There was no evidence of hemosiderin or phagocytized red blood in the membranes, nor any cause of hemorrhage seen grossly in the placenta, e.g. velamentous vessels, or chorionic vessel aneurysm, making hemorrhage external into the amnion space or vagina unlikely. There was no maternal blood test for fetal blood in the mother. Since her blood count had no nucleated red cells, it is unlikely that there was any recent hemorrhage since the fetus had approximately 25% of his red cells nucleated. Against fetal maternal hemorrhage is the intensity of the erythroblastosis, the splenomegaly, and most strongly the hemosiderin in the spleen.
2. Infection: Parvo virus is the most likely cause of relatively acute anemia, but there was no evidence for that infection, and there should have been if it was present. There was no evidence of other fetal infection.
3. Hemoglobinopathy: I have no personal experience with Barth’s hemoglobin, but I would not expect it to have evidence of the short duration of hydrops seen in this infant. The patient is Afro-American and there was no family history of anemia in the chart, but I can not completely exclude the diagnosis.
4. Hemolysis: The hemosiderin in the enlarged spleen in good evidence of the phagocytosis of injured red cells. The mother is Rh negative, and has had two living children. The mother has type O blood and a recent exposure to type A or B might have produced IgG hemolytic antibodies to a major blood type, or she may have antibodies to a non-Rh blood antigen. The autopsy report recommended testing mother for hemolytic antibodies. The fetal blood type was not obtained, but in theory some red blood cell antigens may be detectable on the placental tissue sections. The fetal cells were extremely autolytic, but the maternal blood flow of the placenta maintains some of the red cells despite karyorhexsis.
Tentatively, the final diagnosis is hemolytic disease of unknown cause with a short duration of fetal hydrops and anemia. I would appreciate any comments or help with this case.
1. Fujikura, T. and L. Froelich, Organ-weight/brain -weight ratios as a parameter of prenatal growth: A balanced growth theory of visceras. Am J Obstet Gynecol, 1972. 112: p. 896-902.
2. Genest, D.R., M.A. Williams, and M.F. Greene, Estimating the time of death in stillborn fetuses: I. Histologic evaluation of fetal organs; an autopsy study of 150 stillborns. Obstet Gynecol, 1992. 80: p. 575-84.
Leave a comment